©2022 Saratoga Photographer.com
By Susan Elise Campbell
When Manuel Astruc, M.D., expanded his psychiatric practice years ago from a solo office to one with four nurse practitioners and specialists, he said “the pattern shift would have a bigger impact on the mental health of the community.”
Now Astruc has introduced a new modality, the first in Saratoga County, that he believes will have the same positive effect. The little-known TMS technology he has acquired has been FDA approved for more than 10 years.
“Mental health in the workplace and the impact of depression on company production is a problem,” he said.
According to the Center for Disease Control, “the percent of physician office visits with depression indicated on the medical record is 10.6” and “the percent of emergency department visits with depression indicated on the medical record is 11.2.”
“Even medical professionals and therapists don’t know it’s available,” said Astruc, who has lived and practiced in the Saratoga area for more than 26 years.
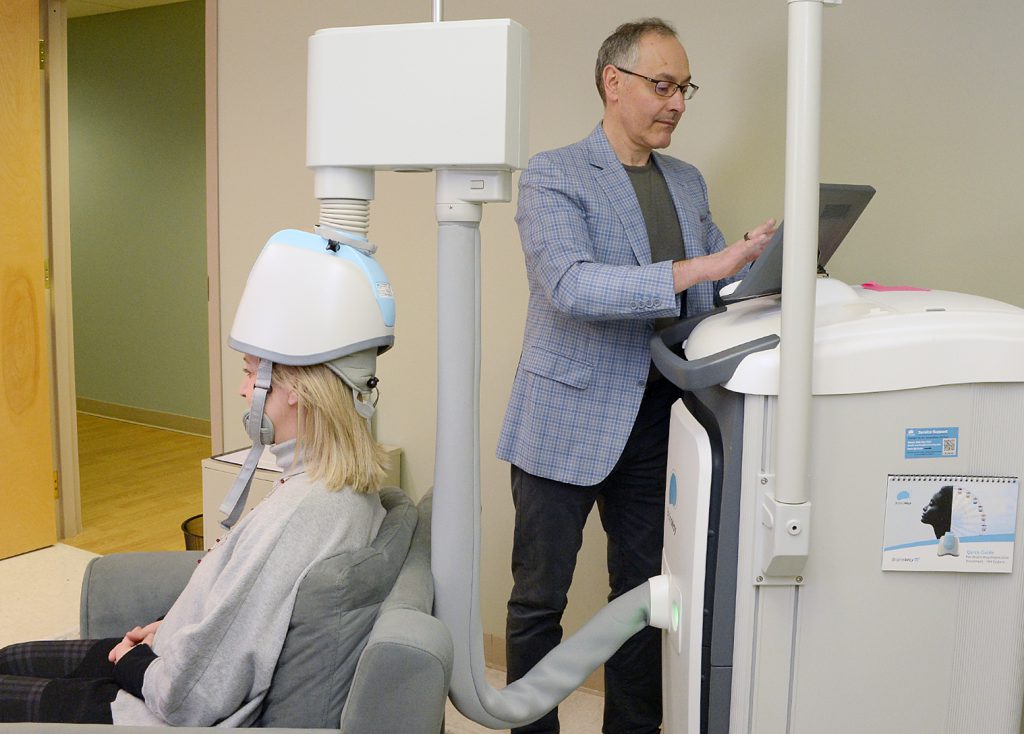
TMS stands for Transcranial Magnetic Stimulation, a machine that stimulates deep areas of the brain and “advances the treatment of mental health disorders without medications or side effects,” he said.
One reason many sufferers of depression, obsessive-compulsive disorder and addiction have been unaware of the existence of TMS therapy is because it is expensive to bring into a psychiatric practice and costly to use in terms of time and manpower, according to Astruc.
“The typical course of treatment takes four to six weeks with five visits per week,” said Dr. Astruc. “That is time-intensive for the practice as every-day visits put demands on staff.”
Moreover, other protocols must be followed in order for health insurance carriers to cover high treatment costs, according to Dr. Astruc.
“FDA says a patient has to have failed out of one medication in order to use TMS in an approved fashion,” he said. And insurance companies can impose other requirements before they will begin to pay for TMS therapy—and then only for severe cases, he said.
“Their protocols vary,” said Dr. Astruc. “These may include two to four medical trials in addition to one or two courses of psychotherapy” all of which must be shown not to have worked.
“This is the world we live in,” he said. “TMS is the next modality, but the failed protocols must first be documented by the insurance company.”
Before TMS, a patient would have to be unresponsive to electroconvulsive (ECT) therapy, which dates back to the 1930s in Europe. This was first used in the U.S. in the early 1940s, Astruc said, when “psychiatric hospitals were the size of cities because there was no treatment for these patients. ECT requires inpatient hospitalization for two to four weeks and the shock is administered three times a week,” he said. “It is referred to as ‘shock therapy’ and while scary, it is effective.”
“That is a long time to be away from family and work,” he said. “With TMS, patients are relieved to hear there is a non-invasive option that is less intense, better tolerated, and does not require hospitalization.”
One side effect of shock therapy is that patients could have a seizure hours or days after the shock was administered, which is why patients were treated in hospital, Dr. Astruc said.
“It is possible for a TMS patient to seizure as well, but it would happen while the stimulation was going on, not later in the parking lot,” he said. “So the doctor can address the situation immediately by turning off the machine until seizing stops.”
Astruc said such a risk is rare. Only one in 10,000 patients are affected in this way.
There is no pain associated with treatment. Instead, patients have a sensation “like a woodpecker tapping on their head, but they get used to it quickly,” he said.
As TMS became widely accepted by insurance, it “made more sense to offer this treatment to patients who were not responding to medications,” he said.
Depression is the primary diagnosis being treated with TMS. Depressed patients feel helpless and hopeless as they struggle to cope with life. Astruc said insurance companies “require the patient to have a severe episode such that they can barely function, but the insurer still can decide whether to cover TMS therapy. Patients can try one more drug and perhaps improve 5 percent,” he said. “But TMS is 50 to 70 percent effective.”
Astruc said there are genetic and environmental influences behind the incidence of depression and other disorders.
He said an increasingly sedentary society has factored into the incidence of depression and the COVID pandemic has amplified the problem.
“Our brains and our bodies are functioning in a different way without social connection,” said Astruc. “And constant bombardment by negative stimulation doesn’t make us feel good.”
“Stress used to be defined as a physical demand on the body that was transitory,” he said. “A constant low-grade demand on the brain affects the hormones that regulate our bodies. We were not made to function that way.”
Learn about TMS therapy at www.manuelastrucmd.com or on his Facebook page, where there are videos and more information. His 414 Maple Ave., Saratoga Springs, office can be reached at 518-583-7410.
